Worried your dog is hurting and not sure what’s safe?
Get clear, vet-reviewed guidance. No guesswork. No email spam.
Medically reviewed by: Kristy Williams, CVT, CCFT (Specialties: Pet rehabilitation, pain management, photobiomodulation)
Reviewed: [April 2026]
Updated: [April 2026]
This page is part of MedcoVet’s clinical education library on photobiomodulation in veterinary medicine. It is designed to explain safe pain relief for dogs, where medications fit, when human pain relievers are dangerous, how acute and chronic pain differ, and where red light therapy may fit into a broader treatment plan.
Every dog owner dreads seeing their canine companion in discomfort. Whether your dog is recovering from surgery, dealing with an old injury, or slowing down due to arthritis, understanding how to safely manage pain in dogs can make the difference between suffering and quality of life. This guide covers everything from vet-prescribed medications to natural alternatives like red light therapy, giving you a complete toolkit for helping your dog feel better.
For a broader overview of pain in dogs, including how red light therapy fits into a full treatment plan, start with our main pain guide.
Worried your dog is hurting and unsure where to start?
Book a free call to get a clear, vet-backed overview of safe pain relief options.
What Can I Safely Give My Dog for Pain Today?

Only veterinarian-prescribed pain medication is safe for dogs. Human painkillers like ibuprofen, Tylenol (acetaminophen), and naproxen are dangerous for dogs and can cause life threatening reactions, even in small doses.
- The fastest safe option: Call your regular veterinarian or a 24/7 veterinary clinic to get an approved canine pain med. Commonly prescribed options include carprofen, Galliprant, or meloxicam, all formulated specifically for dogs.
- Critical warning: Do NOT give human medications like Advil, Motrin, Aleve, Tylenol, or aspirin unless a veterinarian has specifically prescribed them for your dog. Many human pain relievers cause kidney failure, liver failure, and stomach ulcers in dogs. Aspirin and some other medications can also interfere with blood clotting in dogs, increasing the risk of dangerous bleeding. This is why veterinary supervision is essential.
- Vet-prescribed pain relievers for dogs include:
- NSAIDs (nonsteroidal anti inflammatory drugs): carprofen, deracoxib, firocoxib, meloxicam, grapiprant (Galliprant)
- Others: gabapentin, tramadol, opioids (buprenorphine, fentanyl) for further pain releif
- For long-term relief: MedcoVet Luma is a veterinary-grade, at-home red and near-infrared light therapy device that can be added to your dog’s treatment plan. Start with a free clinician consultation to see if it’s right for your situation.
Before you try anything else, check what’s safe for your dog
Human pain meds can cause real harm. This quick quiz helps you understand when red light therapy is a safe option, and when it’s not.
Gideon
Pain relief for dogs depends on diagnosis, not guesswork
Pain relief for dogs is not one-size-fits-all. The right plan depends on whether your dog is dealing with acute injuries, chronic conditions, nerve pain, post-surgical pain, pain and inflammation, or severe pain requiring urgent care. In veterinary medicine, safe dog pain management starts with proper diagnosis, a physical exam, and when needed, blood tests, imaging, and properly prescribed medications under veterinary guidance.
Understanding Pain in Dogs (Acute vs. Chronic)

Not all pain in dogs is the same. Understanding whether your dog is dealing with acute pain or chronic pain helps determine the right approach to treat pain effectively.
- Acute pain is sudden and typically results from trauma, surgery, or a specific incident—a torn cruciate ligament, a fresh wound, or a fall. This type of pain usually lasts days to a few weeks and requires immediate intervention to control pain while healing occurs.
- Chronic pain is ongoing discomfort lasting more than three months. It’s often linked to conditions like osteoarthritis (which affects approximately 20% of dogs over one year old), hip or elbow dysplasia, intervertebral disc disease (IVDD), or long-standing back issues. If you suspect chronic pain in your dog, it is important to have a veterinarian assess and diagnose the condition so they can develop an individualized treatment plan tailored to your dog’s ongoing needs.
- Why untreated pain matters: Dogs that live with unaddressed pain experience slower healing, muscle loss, behavior changes, anxiety, poor sleep, and reduced mobility. Pain isn’t just uncomfortable—it actively harms your dog’s health.
Pain Type | Goal of Treatment | Timeline |
|---|---|---|
Acute Pain | Rapid relief and protection while healing | Days to weeks |
Chronic Pain | Long-term management and quality of life | Ongoing |
- Emergency situations: Any sudden, severe pain—crying out, inability to stand, dragging limbs—requires same-day veterinary care. Don’t wait to see if it improves.
If you want the full condition-level overview of pain in dogs, including when red light therapy helps and when veterinary evaluation should come first, visit our main pain pillar.
Recognizing the Signs Your Dog Is in Pain
Many dogs instinctively hide pain, a survival behavior inherited from their wild ancestors. This means behavior changes are often the first clue that something is wrong.
Behavioral signs to watch for:
- Restlessness or pacing at night
- Hiding or unusual clinginess
- Irritability or growling when touched
- Changes in sleep patterns or decreased appetite
- Reluctance to be petted in certain areas
Movement-related signs:
- Limping or favoring one leg
- Stiffness when getting up, especially after rest
- Reluctance to jump into the car or onto furniture
- Avoiding stairs they previously climbed easily
- Slowing down on walks or lagging behind
Physical signs:
- Panting at rest (not related to heat)
- Trembling or shaking
- Hunched back or tense abdomen
- Pinned ears or squinting eyes
- Excessive licking or chewing at a specific joint or paw

Real-world example: Consider a 9-year-old Labrador who now hesitates before climbing onto the couch, sleeps more during the day, and seems stiff after lying down. These subtle shifts are classic early arthritis clues, easy to dismiss as “just getting older” but worth investigating.
If pain behaviors persist more than 24 hours or worsen, contact your dog’s vet for assessment and a tailored pain plan.
Veterinary Pain Medications for Dogs
Veterinary medicine offers several medication classes for dog pain management, often used in combination to control pain safely while monitoring for adverse reactions. Advances in veterinary science have led to safer and more effective pain management protocols for dogs. Proper monitoring is essential, especially for dogs with existing conditions.
All medications in this section must be prescribed or approved by a veterinarian, with the choice of medication and dosage tailored to your dog’s specific condition, symptoms, and overall health. There’s no safe “one-size-fits-all” approach.
Overview of medication categories:
- Opioids address short-term severe pain
- Drugs like gabapentin target nerve pain or chronic conditions
Routine blood tests and proper monitoring are critical for long-term medication use, especially in older dogs or those with kidney disease or compromised liver function.
Medications can also be combined with non-drug therapies like red light therapy to reduce reliance on higher drug doses over time—always under veterinary guidance.
NSAIDs for Dogs (Vet-Approved Anti-Inflammatories)
Nonsteroidal anti inflammatory drugs reduce pain and inflammation in joints, soft tissue, and after surgery by inhibiting enzymes that produce inflammatory compounds. They’re typically prescribed for mild pain to moderate discomfort.
FDA-approved NSAIDs for dogs:
Medication | Common Use |
|---|---|
Carprofen (Rimadyl, Vetprofen) | Widely used for osteoarthritis and post-op pain |
Deracoxib (Deramaxx) | Often prescribed after orthopedic surgery |
Firocoxib (Previcox) | Used for arthritis and soft-tissue pain |
Meloxicam (Metacam) | Liquid option, sometimes preferred for smaller dogs |
Grapiprant (Galliprant) | Newer class (EP4 antagonist) with different side-effect profile |
Common side effects requiring immediate attention:
- Vomiting or diarrhea
- Decreased appetite
- Black or tarry stools
- Increased thirst or urination
Stop the medication and call your vet immediately if these appear.
Baseline and periodic blood work (every 6–12 months for chronic conditions) helps monitor liver function and kidney health. This is especially important for senior dogs.
Never combine vet NSAIDs with aspirin or another anti inflammatory drugs unless specifically directed by a veterinarian. This dramatically increases the risk of stomach ulcers and serious complications.
Important: Human NSAIDs like ibuprofen and naproxen are NOT the same as veterinary NSAIDs. They metabolize differently in dogs and are dangerous even at low doses.
Opioids and Other Prescription Pain Relievers
Opioids and similar drugs are reserved for moderate to severe pain, often after surgery, trauma, or with advanced cancer. These are effective medications but require careful oversight.
Common opioids used in veterinary practice:
Medication | Typical Use |
|---|---|
Morphine, hydromorphone | Hospital-use for acute, severe pain |
Fentanyl | Often given as a patch post-surgery for continuous relief |
Buprenorphine | Moderate pain, dental or soft-tissue procedures |
Butorphanol, codeine | Select cases or combination protocols |
Side effects to monitor:
- Sedation and drowsiness
- Panting or restlessness
- Nausea and constipation
- Behavior changes
Due to controlled-substance regulations, these require careful dosing and veterinary instructions.
Gabapentin is a common add-on for nerve-related conditions like IVDD, chronic spinal issues, or certain arthritis presentations. While used off-label, it’s widely accepted in veterinary practice for managing nerve pain.
Tramadol is used less commonly now due to questions about its effectiveness in dogs. When prescribed, it’s typically part of a multimodal plan rather than a standalone treatment.
Steroids like prednisone sometimes reduce severe inflammation (spinal swelling, immune-mediated disease) but should never be combined with NSAIDs due to high risk of GI bleeding and ulcers.
Medications help. Long-term plans matter.
Many pet parents use red light therapy alongside meds to support healing and reduce flare-ups over time. Learn how to choose a device that actually delivers a therapeutic dose.
Matilda
Why Human Pain Meds Like Tylenol and Advil Are Unsafe for Dogs
Most human over-the-counter pain relievers are dangerous for dogs—even at low doses. What helps you can seriously harm or kill your pet.
Ibuprofen (Advil, Motrin) Dogs lack the enzymes to process ibuprofen safely. Even one pill can cause stomach ulcers, intestinal bleeding, and kidney failure. Larger doses can be fatal.
Naproxen (Aleve) Similar to ibuprofen but with an even longer half-life in dogs, meaning toxic effects last longer. Causes severe gastrointestinal damage and kidney damage.
Acetaminophen (Tylenol) Causes liver failure and damages red blood cells. Small breeds are especially vulnerable. Signs of toxicity include facial swelling, brown-colored gums, and labored breathing.
Aspirin While occasionally prescribed by veterinarians at carefully calculated doses, aspirin causes GI ulcers and bleeding issues in dogs. It’s not a safe DIY option without proper dosage guidance from your vet.
Signs of toxicity to watch for (may appear within hours to days):
- Vomiting (possibly with blood)
- Black, tarry stools
- Lack of appetite
- Increased thirst and urination
- Jaundice (yellowing of eyes or gums)
- Lethargy or collapse
If you’ve already given a human pain med: Contact your vet immediately, a pet poison hotline, or emergency veterinarian right away. Have the exact drug name, strength, amount given, and time available.
There is no “safe at-home dose chart” for human pain pills. All dosing for human pain meds must be prescribed by a veterinarian for your individual dog—giving your dog even a fraction of a human dose can cause severe organ damage.
Safety is First
Red light therapy offers drug-free pain support without stressing the liver or kidneys. See how it works and when it’s appropriate.
Huxley
Natural and At-Home Pain Relief Options (Including Red Light Therapy)

Non-drug therapies can be remarkably effective for chronic pain and are often used alongside appropriate medications to improve comfort and potentially reduce drug doses over time.
Simple home strategies:
- Controlled rest during flare-ups
- Non-slip rugs or runners on slick floors
- Ramps for beds, couches, and vehicles (use a ramp to get into the SUV instead of jumping)
- Raised food and water bowls to reduce neck strain
- Orthopedic dog beds with memory foam support
- Maintaining a healthy weight through portion control
Low-impact exercise options:
- Short, controlled leash walks
- Underwater treadmill sessions (with professional guidance)
- Swimming in warm water (supports joints while building muscle)
- Physical therapy exercises prescribed by a veterinary rehab specialist
Validated alternative therapies:
- Acupuncture (studies show 65% pain reduction in hip dysplasia cases)
- Massage therapy to relieve muscle tension
- Heat therapy for stiff muscles and joints
- Joint supplements including glucosamine, chondroitin, omega-3 fatty acids, UCII (type II collagen)
- Adequan injections for joint disease
Red light therapy (photobiomodulation) stands out as a leading non-invasive, drug-free option for long-term pain control. It’s particularly effective for arthritis, joint pain, IVDD, hip dysplasia, muscle strains, and post-surgical healingwithout the side effects of medications.
If you want results, dosing matters
This short class explains how red and near-infrared light reduce pain, why timing matters, and what most home devices get wrong.
Mizzy
What is PBM and how does it fit into dog pain management?
Photobiomodulation, also called PBM, red light therapy, low-level laser therapy, LED therapy, cold laser, and near-infrared therapy, refers to the same therapeutic category using light energy to influence cellular biology. In veterinary medicine, PBM is used to help manage pain, reduce inflammation, support blood flow, and promote tissue repair. In dogs, it is often used for chronic pain, joint pain, nerve pain, acute injuries, post-surgical healing, and broader dog pain management as part of a multimodal treatment plan.
Red Light Therapy for Dog Pain Relief (How It Works)
Red and near-infrared (NIR) light therapy has been used in human and veterinary medicine for decades to reduce inflammation, relieve pain, and support tissue healing. It’s gaining significant traction as dog owners seek natural supplements to pharmaceutical approaches.
The science in simple terms: Red and NIR light at specific wavelengths (typically 600-1000nm) penetrates the skin and is absorbed by mitochondria—the energy centers of cells. This triggers increased ATP (cellular energy) production and activates anti-inflammatory and pro-healing processes at the cellular level.
Key therapeutic effects:
- Reduced joint inflammation and swelling
- Decreased stiffness and improved range of motion
- Enhanced blood flow to damaged tissues
- Faster soft-tissue repair
- Improved mobility and comfort over time
For a deeper review of wavelength selection, dosing logic, safety, tissue depth, and device considerations, see Science of Red Light Therapy.
Why it’s ideal for long-term use: Unlike many medications for dogs, properly used light therapy doesn’t stress the liver function or kidneys. This makes it particularly valuable for senior dogs or those who can’t tolerate higher drug doses due to organ concerns.
Multiple veterinary studies have demonstrated benefits for conditions including osteoarthritis (with 70-90% pain reduction reported in some cases), wound healing, and post-operative recovery.
Light therapy is generally painless—most dogs relax during sessions. Treatment frequency typically starts higher (several times per week) and tapers as the dog improves, with cumulative benefits often lasting months.
For a broader overview of conditions, use cases, and treatment expectations, see Red Light Therapy for Dogs.
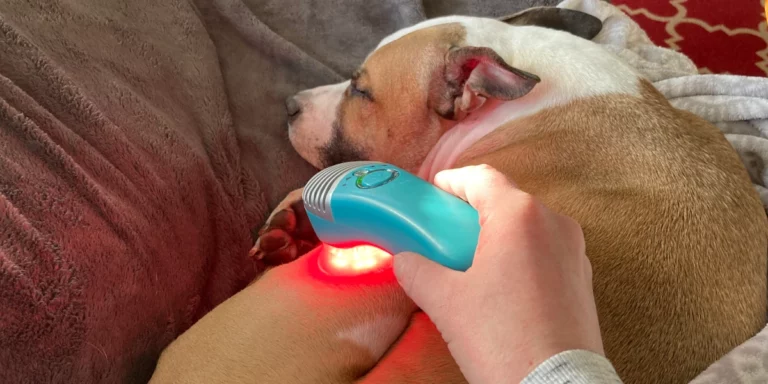
MedcoVet Luma: At-Home Vet-Grade Red Light Therapy

MedcoVet Luma is a home-use, veterinary-grade red and near-infrared light therapy system designed specifically for dogs (and cats) with chronic pain and mobility issues. It’s the same technology trusted by 250+ veterinary clinics, now available for convenient at-home treatment.
Key technical features:
- Uses clinically relevant 635nm (red) and 850nm (near-infrared) wavelengths—the same used in professional veterinary rehab clinics
- Delivers consistent, therapeutic doses across the treatment area
- Specialized comb technology allows effective light delivery even through thicker or long coats
- Portable design for treating joints, muscles, and spine
Conditions Luma addresses:
- Arthritis (hips, knees, elbows, spine, shoulders, hocks)
- Joint pain from dysplasia
- IVDD and back pain
- Cruciate ligament disease (pre- and post-surgery)
- Muscle strains and tendon injuries
- Post-surgical incision healing
- Otitis and other inflammatory conditions
The MedcoVet care model:
- Free online clinician consultation to assess your dog’s specific condition
- Personalized treatment protocol based on diagnosis and history
- Ongoing support via app and messaging while you treat at home
- Proper diagnosis guidance to ensure appropriate use
Benefits for pet parents:
- Non-invasive and drug-free
- No sedation required
- Treat at home on your schedule
- Reduces need for frequent (and expensive) in-clinic laser sessions
- Natural pain relief without worrying about organ side effects
Let a clinician review your dog’s case
Get a personalized protocol based on your dog’s condition, size, coat, and history. Free. No pressure.
Ella
How to Comfort a Dog in Pain at Home (Day-to-Day Management)
Medications and therapies work best when combined with thoughtful day-to-day management at home. Small adjustments can make a significant difference in your dog’s comfort.
Environment adjustments:
- Create a quiet, draft-free resting area away from household traffic
- Use thick, supportive bedding that cushions joints
- Keep food and water close to minimize painful movement
- Ensure easy access to potty areas without navigating stairs
Flooring and mobility support:
- Place non-slip runners or rugs in hallways and on slick surfaces
- Use yoga mats in areas where your dog stands frequently
- Install ramps or pet steps for accessing couches, beds, and vehicles
- Consider a supportive harness or sling for dogs with back leg weakness
Weight management: Even a few extra pounds dramatically strain joints. Work with your dog’s vet to develop a weight-loss plan if needed—measured portions, appropriate calorie intake, and gentle exercise all contribute. Studies consistently show that maintaining healthy weight is one of the most impactful ways to manage chronic pain.
Mental well-being matters too: Just because long hikes are off the table doesn’t mean enrichment should stop. Try some of the following enrichment activities:
- Scent games and nose work
- Puzzle feeders and food-dispensing toys
- Gentle training sessions with low-impact tricks, which are often recommended for dogs recovering from IVDD (intervertebral disc disease)
- Quality time with calm petting and massage
Keep a pain diary: Track date, activity level, pain signs observed, medications given, and any light therapy sessions. Share this log with your vet or MedcoVet clinician to fine-tune the treatment plan over time.
Ghillie
Want help dialing this in?
Bring your notes, your questions, and your goals. A MedcoVet clinician will help you build a plan you can start right away.
When to SVet (or Emergency Clinic) for a Dog in Pain
While home supports and therapies are valuable, certain signs require prompt veterinary attention. Knowing when to act can save your dog’s life.
Emergency red flags (seek immediate care):
- Inability to stand or walk
- Sudden paralysis or dragging legs
- Continuous crying, screaming, or yelping
- Swollen or obviously broken limb
- Severe abdominal pain (tense belly, restlessness, vomiting)
- Pale mucus membranes
- Trauma (hit by car, major fall) even if the dog seems “okay”
- For pets with underlying conditions, such as hypertension, sudden severe symptoms may require immediate veterinary attention.
Urgent signs requiring same-day or next-day care:
- New or worsening limp
- Refusal to walk or move
- Reluctance to jump lasting more than 24 hours
- Repeated vomiting with signs of pain in the same day
- Pain not controlled by current pain meds
- Any adverse reactions to medications
Before traveling to the vet:
- Call ahead to alert them you’re coming
- Limit your dog’s movement to prevent further injury
- Use a sling or towel to support back legs if needed
- Avoid manipulating obviously painful areas
- Keep your dog calm and comfortable during transport
Bring with you:
- List of all medications (including natural supplements, CBD, any other medications)
- Any human meds accidentally given (with exact drug, strength, and time)
- Your pain diary or home-tracking notes
The combined approach works best: veterinary guidance + properly prescribed medications + non-invasive tools like MedcoVet Luma + thoughtful home care = the best chance at a comfortable, active life for dogs living with acute and chronic pain.
Key Takeaways
- Only vet-prescribed pain meds are safe for dogs—human pain relievers like ibuprofen and Tylenol can cause kidney failure, liver failure, and death
- Learn to recognize subtle pain signs since dogs often hide discomfort
- NSAIDs and opioids serve different purposes and require proper monitoring with regular blood tests
- Natural options like physical therapy, joint supplements, and red light therapy can reduce medication needs
- MedcoVet Luma brings veterinary-grade light therapy home, making consistent treatment accessible for chronic conditions
- Day-to-day management (weight control, environment adjustments, mental enrichment) amplifies the benefits of any pain plan
Your dog depends on you to recognize when something’s wrong and to find safe, effective solutions. Whether you’re managing acute injuries or helping your senior pup stay comfortable through their golden years, the right combination of veterinary care and at-home support makes all the difference.panion’s specific needs.
You don’t have to figure this out alone
If your dog is dealing with pain, there’s a safe next step. Get expert guidance and see if red light therapy fits your dog’s needs.
Clinical summary
Mechanism:
Pain relief for dogs depends on identifying the source of pain and matching treatment to the biology involved. Pain medications may reduce pain and inflammation through anti inflammatory drugs, modulation of nerve signaling, or central pain control. Photobiomodulation may support mitochondrial activity, ATP production, inflammatory signaling, blood flow, and tissue recovery.
Evidence level:
Evidence is strong for appropriately prescribed NSAIDs and other commonly prescribed medications in selected pain states, especially osteoarthritis, post-surgical pain, and inflammatory conditions. Evidence for photobiomodulation is moderate to strong in selected musculoskeletal and inflammatory conditions, particularly osteoarthritis, soft tissue injury, and post-operative recovery. Evidence varies by diagnosis, tissue depth, treatment frequency, and overall treatment plan.
When it works best:
A multimodal approach works best for acute and chronic pain, including joint pain, osteoarthritis, hip dysplasia, soft tissue injury, post-surgical recovery, and some forms of nerve pain. In many dogs, the most effective pain control comes from combining properly prescribed medications, physical therapy, environmental changes, weight management, and non-drug tools such as PBM.
When not to use:
Human pain meds, human pain pills, and many human pain relievers should not be used unless explicitly directed by a veterinarian. Photobiomodulation should not be used casually when proper diagnosis is missing, when severe trauma or fracture is suspected, when major neurologic decline is present, when untreated infection is suspected, or when an unexplored mass or tumor may be present in the treatment area.
Limitations:
Pain relief does not replace diagnosis. Even effective medications can cause adverse reactions, kidney disease complications, liver function concerns, blood clotting issues, stomach ulcers, increased thirst, decreased appetite, or other serious complications if the medication, proper dosage, or proper monitoring are wrong for the dog’s specific condition. PBM is not a replacement for surgery when surgery is indicated, nor for emergency care in a dog with severe pain.
Clinical questions pet owners ask about pain relief for dogs
Evidence Citations

About the Author
Alon Landa is the CEO and co-founder of MedcoVet, a leader in at-home red light therapy for pets. With over 20 years of experience in medical technology and firsthand involvement in developing the Luma, Alon combines deep technical knowledge with a passion for improving pet health. He regularly collaborates with veterinarians and pet parents to advance photobiomodulation (PBM) care at home.
📍 Based in Boston, MA
📖Read more from Alon here

About the Medical Reviewer
Clinical Focus: Surgery, anesthesia, canine fitness, injury prevention, agility
Kristy Williams brings over 30 years of experience to the veterinary field. Her career began in the 1990s, working as a civilian for the Army Veterinary Corps at RAF Feltwell in England, where she first discovered her passion for animal care and supporting their families. Upon returning to the United States, Kristy pursued her education and graduated in 2005 as a certified veterinary technician after passing the national exam. She has since gained extensive experience in both general practice and emergency/referral practices.
Read More about Kristy here.
🐾 Ready to Take the Next Step?
Whether you’re just learning or ready to act — we’ve got you.
👉 Book a Free Consult
Talk to a licensed clinician about your pet’s condition and get a personalized plan. No pressure, just real help.
👉Learn More About the Luma
Explore how our at-home red light therapy device works, why it’s different, and what it can do for your pet.